[Parent Connection] Bone Health Part 1: Peak Bone Mass
One in three women and one in five men over 50 years old will suffer from an osteoporotic fracture sooner or later in their lives1. And among the 10,000 hip fracture cases each year in Hong Kong, one-fifth pass away within the year and half of them sustain permanent mobility impairment1. Osteoporosis is unquestionably a public health concern among older adults.
But little do most people know, the prevention of osteoporosis starts early in childhood.
How? Let’s jump right into today’s topic: Peak Bone Mass.

What is “Peak Bone Mass”?
Our skeleton grows as our body grows. A human is typically born with about 300 soft bones. Over time and influenced by a myriad of intrinsic and extrinsic factors, these soft bones are replaced by hard bones, and eventually, fused into a 206-bone adult skeleton. Peak bone mass refers to the amount of bones developed when the skeletal state achieved stability. Generally speaking, total skeletal mass usually peaks at age 26 to 30 while certain parts, such as the skull, continue to grow throughout life. Thereafter, bone mass will not increase anymore and is maintained by bone remodeling (e.g. replacing old bone tissues with new ones). As we age, the rate of bone resorption far excess that of bone formation, hence, here begins the decline of bone mass, and potentially, the common fate of osteoporosis.
Approximately half of our bone mass is accumulated during adolescence. As evidenced by research, a 10% increase in peak bone mass may delay osteoporosis development by 13 years4. That said, maximizing bone mass while young allow us to build a strong foundation to delay, or better, prevent the development of osteoporosis. While the full potential of peak bone mass is genetically programmed in each of us, whether we are able to achieve such optimum depends on various intrinsic and extrinsic (i.e. environmental) factors to be discussed below.

Factors Influencing Peak Bone Mass

Genetics. Extensive research indicates that genetic accounts for 60-70% of the variability in peak bone among individuals. Genes critical to body size and growth hormone regulations are often key influencers of bone mass as well. Some genetical factors may intertwine with environmental factors resulting in specific effects on bone mass. For example, a person with higher efficiency of calcium absorption and utilization by genetics may achieve a higher peak bone mass to his/her slow metabolizer counterparts when both have a usual diet with marginal calcium intake. However, it is important to note that the manipulation of environmental factors can also “change the fate” destined by genetics. Using the same example, the impact of calcium metabolism genetic difference can be minimized simply by adequate intake of calcium.
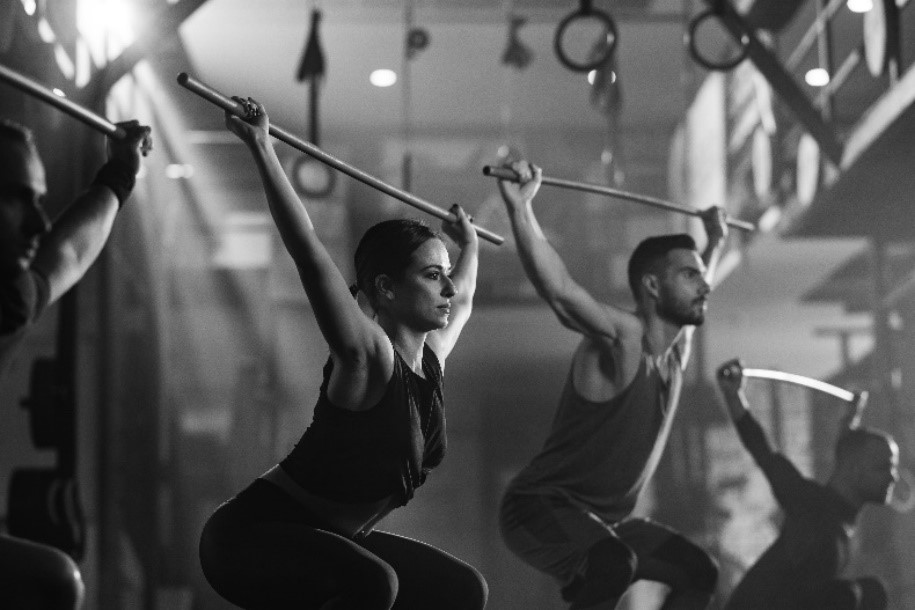
Environmental factors. Adequate nutrition with key nutrients including calcium, protein and vitamin D support various processes contributing to peak bone mass, such as bone matrix production, bone tissue, growth hormone regulation, etc. On the other hand, undesirable dietary patterns, for instance excessive saturated fat intake, may result in opposite effect and hinder bone growth in early life. Weight-bearing exercises, such as stair-climbing and resistance exercises, stimulate bone mass development as weight compresses the bone matrix and triggers the cells to deposit more calcium and other minerals. For this very reason, the World Health Organization has suggested regular physical activity for optimal bone health in children and adolescents. In addition, lifestyle behaviors including alcohol use and tobacco use have been associated with lower peak bone mass in young women and men9-11.
In summary, there are ways to outrun genetics and achieve the full potential of your peak bone mass. Stay tuned and we will discuss how you can eat your way to optimal bone health!

References:
- HKSAR. Press Releases. LCQ10: Osteoporosis. Available at: https://www.info.gov.hk/gia/general/201911/20/P2019112000334.htm.
- Heaney R P, et al. Osteoporos Int. 2020;11:985-1009.
- International Osteoporosis Foundation. Bone Biology. Available at: https://www.osteoporosis.foundation/health-professionals/about-osteoporosis/bone-biology.
- Hernandez C J, et al. Osteoporos Int. 2003;14(10):843-847.
- Prentice A. Proc Nutr Soc. 2001;45-52.
- Proia P, et al. Front Endocrinol. 2021. 12:704647.
- International Osteoporosis Foundation. Serve Up. Available at: https://www.osteoporosis.foundation/sites/iofbonehealth/files/2019-03/2015_ServeUpBoneStrengthNutrition_FactSheet_English_0.pdf.
- Weaver C M, et al. Osteoporos Int. 2016;27(4):1281-1386.
- LaBrie J W, et al. J Stud Alcohol Drugs. 2018;79(3):391-398.
- Callréus M, et al. Calcif Tissue Int. 2013;93(6):517-25.
- Taes Y, et al. JBMR. 2020;25(2):379-387.
- Zhu X, et al. Front Med. 2020;doi:10.1007/s11684-020-0748-y.

